The Interactive Quality Measures report provides both summary and detailed information about the quality measures available for CMS reporting for MIPS.
Report Filters
The following filters and parameters allow you to refine the data displayed across all report charts and tabs
Use the View By parameter to select whether to view measures by TIN or by individual Provider/NPI
Select the year for which you wish to view data using the Year filter
There are separate filters for TIN and for Provider Name and NPI

Note: The NPI filter is populated only when the View By parameter is set to NPI.
There are three report tabs available with various tables and charts, as described, below.
MIPS Dashboard
The MIPS Dashboard is the main view and summarizes data into three charts.
The TIN/NPI Measure Summary displays the total number of measures by status category across all TINs/NPIs.
There are five status categories:
Status | Definition | Next Steps |
Insufficient Data | The measure does not meet the minimum reporting criteria, as defined by CMS. For example, for 2018, a measure must have at least 20 cases reported and a Reporting Rate of at least 60%. | Make sure you have reported all possible exams for all patients, including non-Medicare patients. |
Insufficient Data, No Historical Benchmark Available | The measurement does not meet the minimum reporting criteria AND there is no historical benchmark currently available from CMS. | Report additional cases, if possible. |
Reporting Eligible, No Historical Benchmark Available | The measure does meet reporting criteria and is available for reporting to CMS, but there is no historical benchmark currently available. | You can still choose the measure for reporting, but you will receive only the minimum points unless a benchmark is created by CMS later in the year. |
Reporting Eligible, with Benchmark | The measure meets reporting criteria and a benchmark is available. | Select the measure for CMS reporting. |
Selected for CMS | The measure meets reporting criteria, has been benchmarked, and has been selected for reporting to CMS. | Select and finalize your quality measures for CMS submission. |
The Measure Counts bar chart provides the next level of detail with counts of measures in each status category for each TIN or NPI so that you can identify where additional data may be needed to meet reporting criteria.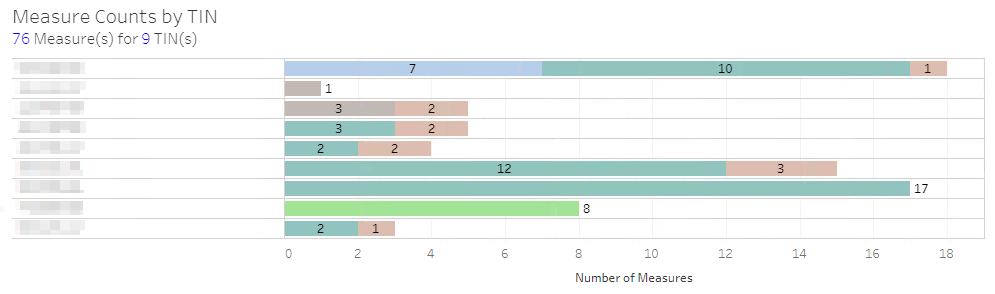
The MIPS Measures Deciles is a visual representation of benchmarked measures, with Deciles on the y-axis and measures on the x-axis.

This chart can help identify patterns such as measures with lots of low deciles or providers with below-average measures. See Interactive Features, below, for how to navigate the data in this chart.
Quality Performance Summary
The Quality Performance Summary provides a high-level view of performance across all MIPS and QCDR measures for each TIN/NPI. The table shows performance scores for Continuous measures and performance rates for Proportional measures, to help identify patterns across measures and TIN/NPIs.
You can download the data from this table by clicking just above the column headers, clicking the Download icon in the lower right corner, and selecting Crosstab.
Quality Measure Detail
This table provides the most detailed information about each measure for TINs/NPIs, using a format similar to the MIPS Performance Report. Measures falling below CMS reporting criteria are highlighted, with indicators in the Reporting Numerator column for measures with fewer than the CMS case minimum, and in the Reporting Rate column for measures with reporting rates below the CMS threshold.

The report has an additional Measure Status filter to restrict the table to specific status categories – e.g. if you want to show only measures with a status of Insufficient Data.
Interactive Features
There are a number of ways to drill down and highlight data, using the MIPS Dashboard, to gain insight into the data.
Using the Measure Summary pie chart, you can identify all measures in a specific status category by hovering over a slice in the chart to display the See All Measures with This Status link. Clicking the link takes you to the Quality Measure Detail tab, which is automatically filtered to show only measures having the highlighted status. For example, clicking on the link in the chart to the left would display detailed data for all 19 measures with status Reporting Eligible, with Benchmark.
You can filter or highlight the MIPS Measure Deciles scatterplot using either the Measure Counts bar chart or the scatterplot legend. Clicking on a bar in the bar chart filters the scatterplot to show only those measures specific to the selected TIN/NPI. Remove the filter by clicking again anywhere on the chart, or by clicking the Undo button in the lower left corner.
Clicking on a TIN / Provider in the scatterplot legend performs a similar function, but rather than completely filtering the chart it highlights the selected TIN/NPI by making all other values fainter as in the example, below. You can also single-click on any mark in the scatter plot to highlight all measures for that TIN/NPI.

Hovering over a mark in the scatterplot displays additional details for that measure, including the measure name, performance score/rate, and CMS benchmark (if available).

ACRad 34 Subcomponents
ACRad 34 was introduced in performance year 2019. This QCDR measure is comprised of previous QCDR measures ACRad 31 – 33.
To help provide some consistency across performance years, the report contains a new Measure Components tab that lists measure components for ACRad 34 for all TINs / NPIs selected from the MIPS Dashboard tab.

You can also access this information using several functions from the other report tabs. On the MIPS Dashboard tab, the details are available from the MIPS Measure Deciles chart when you hover over the ACRad 34 mark.

In the example, above, the table from the Measure Components tab has been filtered to include only the ACRad 34 details because this the mark over which the mouse was placed. This same interactivity is also available when hovering over measures in the Quality Performance Summary tab.
On the Quality Measure Detail page you can click on the ACRad 34 measure to generate a link to the Measure Components tab to see the details for that TIN/Provider and measure.


